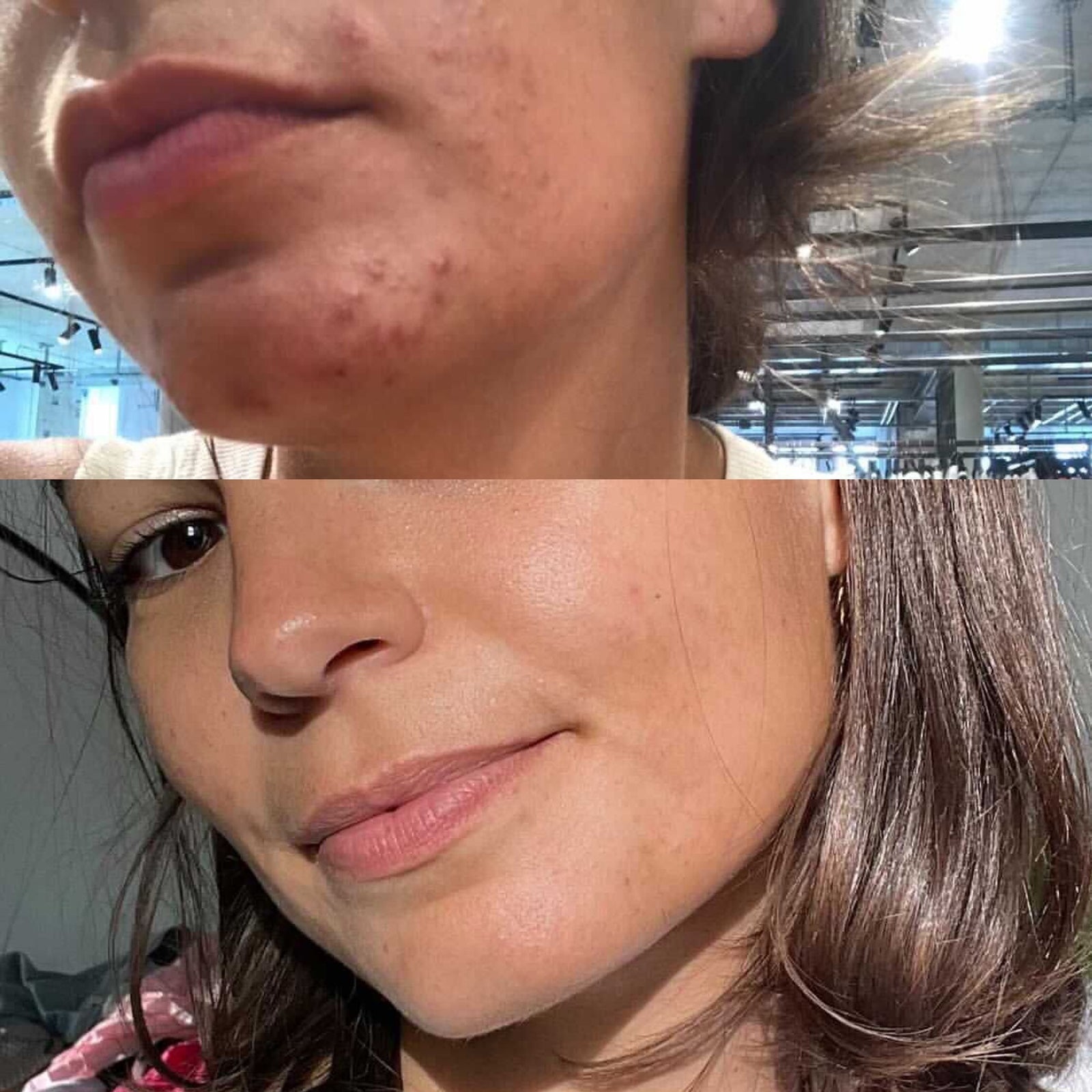
Antibiotic resistance is amongst one of the main causes of treatment failure in acne vulgaris today.
This is due to the excessive use of antibiotics in agriculture, over prescription in humans, and a lack of research on new antibiotics, all slowly contributing to antibiotic resistance. If you want more information how the overuse of Penicillin contributed to the Founder of Klarskin's acne, check out this blog post on the link between liver health and acne.
Globally, P. acnes resistance to antimicrobials has increased almost 40% between the 1980s and 2000s worldwide.
In fact the problem is more serious than we think. Over 2 million Americans become infected every year with antibiotic resistant bacteria, resulting in about 23,000 deaths.
Bacteria is a huge piece of the puzzle relating to all skin issues. In fact research shows that different bacteria causes different kinds of reactions on skin dependant on age and circumstance.
Age related shifts in bacterial communities could explain why certain skin diseases are prevalent at different stages of life. For example, it explains why children are more susceptible to atopic dermatitis, as their microbiome is composed of mostly Streptococcic, Bacteroides, and Proteobacteria.
However when we enter puberty, spikes in androgens lead to a more susceptible environment for the development of acne and a shift in microbiome concentration to greater levels of Propionibacterium and Corynebacterium. This means less atopic dermatitis and more pimples and blackheads, most commonly found in teenagers.
A change in bacteria and hormones ultimately affects what type of acne you may be experiencing, but since bacteria plays such a big role in the formation of acne, antibiotics can be a really effective way of fighting acne.
Overuse of antibiotics, including long-term use of antibiotics, is associated with the development of antibiotic resistance, researchers explain that antibiotic use may lead to the emergence of an antibiotic-resistant form of acne-causing bacteria.
Basically, if you consume antibiotics long term this can promote the formation of an antibiotic resistant biofilm that protects the bacterium against host defences and can alter the natural microbiota of the skin. It is therefore important to support your body in excreting excess biofilm and replenishing your microbiome
How to combat this growing epidemic? Be aware of the importance of your liver health, support your lymphatic pathways, your elimination pathways (gut, colon) and consume foods that aid in the elimination of toxin build up and waste. More on this from us to come so stay tuned!
Reference: Propionibacterium (Cutibacterium) acnes Bacteriophage Therapy in Acne: Current Evidence and Future Perspectives David E. Castillo . Sonali Nanda . Jonette E. Keri, 2018